15 Jan Task Force Releases New Clinical Episode Model Resources
HEALTH CARE TRANSFORMATION TASK FORCE RELEASES CLINICAL EPISODE MODEL RESOURCES
New Tools Support Payers and Providers in Establishing Commercial Value Contracts
WASHINGTON (January 15, 2019) – The Health Care Transformation Task Force (HCTTF or Task Force), a group of leading health care payers, providers, purchasers and patient organizations, today released a set of resources to support effective implementation of clinical episode models in the commercial market.
“These tools will help to simplify the process for payers and providers to develop bundled payment arrangements to drive high-quality, patient-centered specialty care for their patients,” said Dave Terry, CEO of Archway Health and co-chair of the Task Force’s Advanced Payer/Provider Partnerships Work Group. “The promising results from bundled payment initiatives in the Medicare program demonstrate that there is significant potential for clinical episode models to drive cost savings and quality improvements in the commercial market.”
The new whitepaper, Episode Groupers: Key Considerations for Implementing Clinical Episode Models, examines the role of episode groupers within the context of clinical episode payments and offers a framework for decisionmakers to assess various options. The Task Force also released a new contracting guidance document, Clinical Episode Contracting for Commercial Payers, to support payers and providers in launching commercial-sector clinical episode payment arrangements.
“Clinical episode value models are common in both Medicare and several state Medicaid programs,” said Jeff Micklos, Executive Director of the Task Force. “A significant opportunity for uptake of these models in commercial markets remains.”
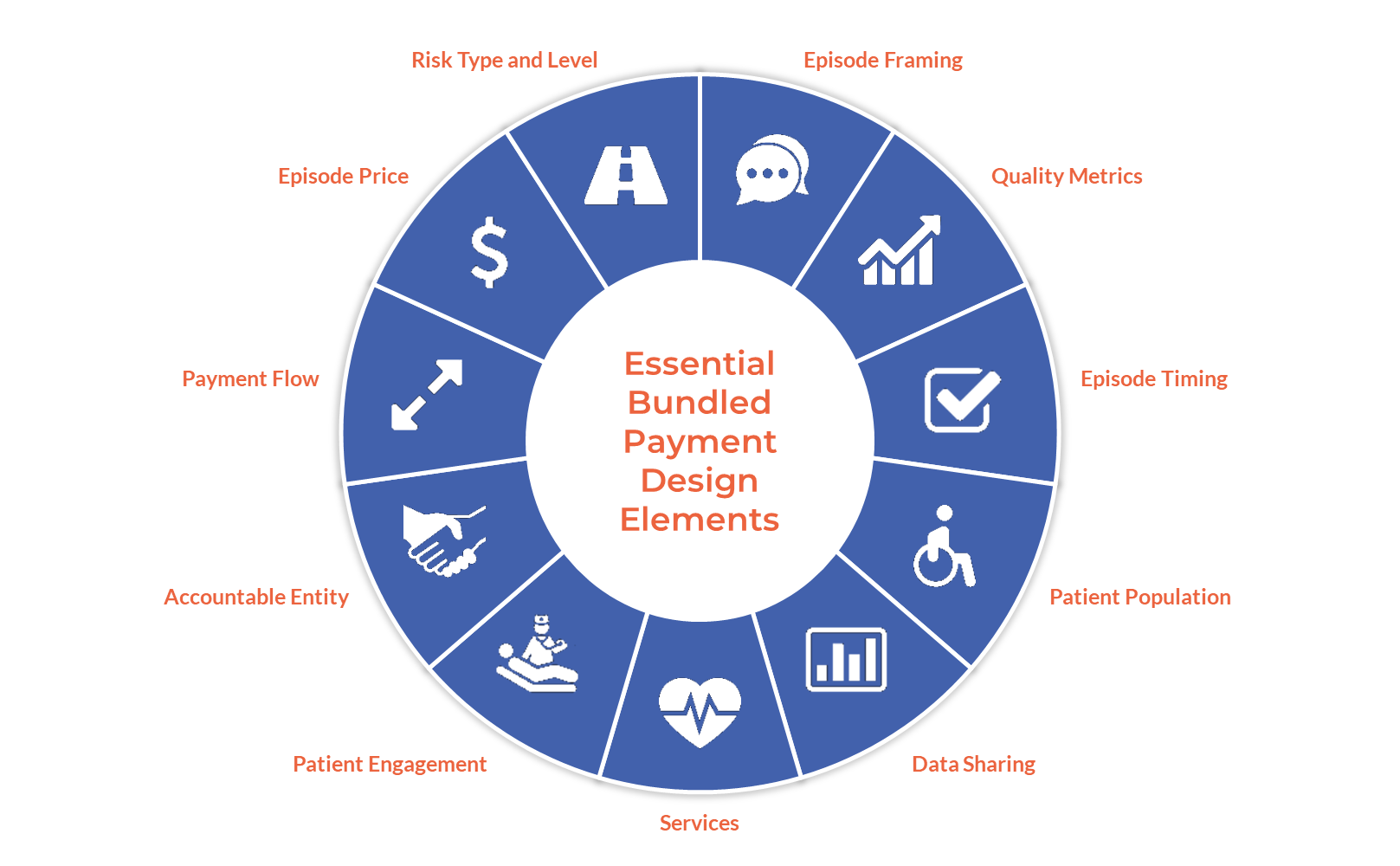
“We see bundled payments as a crucial mechanism to engage specialists in value-based care delivery,” said Erin Smith, Director of Payment Innovation at Anthem, Inc. “Working from a common framework of essential bundled payment design elements helps us in establishing strong relationships with our provider partners.”
The development of these resources was overseen by the HCTTF Advanced/Payer Provider Partnerships Work Group, which serves as a forum for vanguard organizations to discuss the “future state” needs for value-based payment arrangements and share lessons learned by organizations trying to scale advanced payment models.
The resources build upon the bundled payment framework developed by the Health Care Payment Learning and Action Network (LAN) to provide implementation-focused design elements and operational considerations for episode payment models to succeed.
For more information please visit: www.hcttf.org.
ABOUT THE HEALTH CARE TRANSFORMATION TASK FORCE
The Health Care Transformation Task Force is a unique collaboration of patients, payers, providers and purchasers working to lead a sweeping transformation of the health care system. By transitioning to value-based models that support the Triple Aim of better health, better care and lower costs, the Task Force is committed to accelerating the transformation to value in health care.
TASK FORCE MEMBERS
Aetna • agilon health • Aledade • American Academy of Family Physicians • Anthem, Inc. • ApolloMed • Archway Health • Ascension • Atrius Health • Blue Cross Blue Shield of Massachusetts • Blue Cross Blue Shield of Michigan • Blue Cross Blue Shield of North Carolina • Blue Cross Blue Shield of South Carolina • CareCentrix • ChenMed • Clarify • Cleveland Clinic • Community Catalyst • ConcertoHealth • Dignity Health • Encompass Health • Evolent Health • Geisinger • HRHCare • Kaiser Permanente • Mark McClellan • National Health Law Program • National Partnership for Women & Families • OSF HealthCare • Pacific Business Group on Health • Partners Healthcare • patientping • Premier • Remedy Partners • SCL Health • Sentara Healthcare • Trinity Health • True Health New Mexico • Tucson Medical Center • Washington State Health Care Authority • UAW Retiree Medical Benefits Trust
