24 Sep 2018 Transformation Progress Report
Health Care Transformation Task Force Announces Increase in Value-Based Arrangements
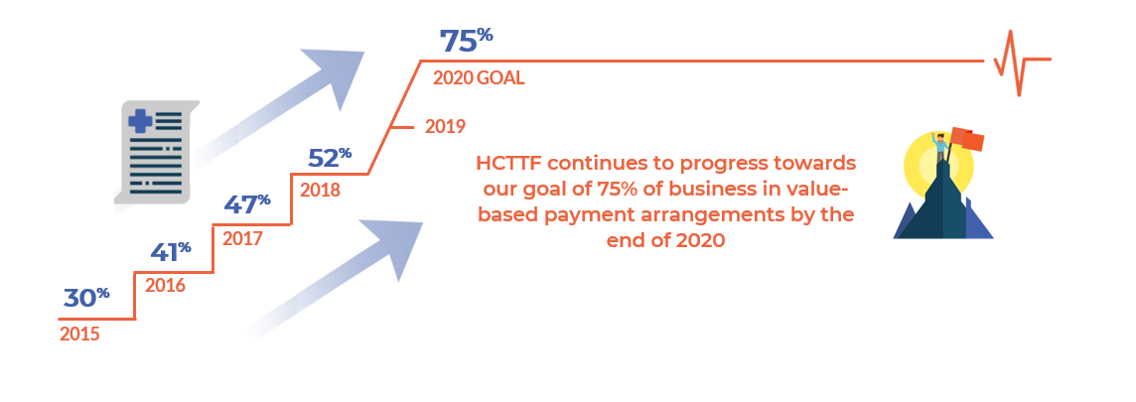
WASHINGTON (September 24, 2019) – The Health Care Transformation Task Force (HCTTF or Task Force), a group of leading health care payers, providers, purchasers and patient organizations, today released a report announcing that its provider and payer members had over half (i.e., 52 percent) of their business in value-based payment arrangements at the end of 2018.
The Task Force and its members aspire to have 75 percent of their respective businesses operating under value-based payment arrangements by the end of 2020. These arrangements focus on lowering costs and improving the quality of care and overall population health. The new report shows progress towards the goal and has increased substantially from the group’s first report of 30% in value-based arrangements in 2015.
“Task Force members have made important and impressive progress in moving the dial on value-based payment adoption,” said Fran Soistman, Executive Vice President and Head of Government Services with Aetna, A CVS Health Company and HCTTF Chair. “HCTTF members are delivering on their commitment to moving health care delivery away from fee-for-service to innovative payment models that foster high-quality, patient-centered care.”
“As our members advance in value-based payment models, Task Force members continue to note obstacles that hinder industry progress in transitioning to value,” said Jeff Micklos, Executive Director of HCTTF. “While many Task Force members have achieved the 75 percent goal already, many willing organizations are finding it difficult to reach that threshold for various reasons.”
The Task Force defines value-based payment arrangements as those that “successfully incentivize and hold payers and providers accountable for the total cost, patient experience, and quality of care for a population of patients, either across an entire population over the course of a year or during a defined episode that spans multiple sites of care.”
In addition to reporting on its annual progress, the Task Force serves as an industry convener and a leading public voice on value-based payment and care delivery transformation by developing resources and perspectives that promote effective value-based payment and care delivery and public policies. This year, the Task Force released the following tools available to the public to aid in the health care system’s transformation:
• Value Partnership Evaluation Tool, an interactive tool to support leaders as they assess potential partner organizations – or themselves – for readiness to engage in successful value-based partnerships, designed around a set of core competencies.
• Consumer Engagement in Benefit Design Principles, a set of principles to guide payers, purchasers, and providers in their efforts to better integrate consumer needs and preferences into insurance benefit design, and Engaging Consumers in Care Delivery, an implementation framework and set of best practices organizations to evaluate existing efforts and support new consumer engagement initiatives.
• Episode Groupers: Key Considerations for Implementing Clinical Episode Models, which examines and evaluates episode groupers and clinical episode payment approaches, and Clinical Episode Contracting Guidance for Commercial Payers, an objective tool for payers and providers to work together to make key program and contract design decisions on episode payment models.
• Expanding Access to Outcomes-Driven Maternity Care Through Value-Based Payment, a comprehensive report highlighting evidence in support of payment reform models to improve maternal health outcomes.
The transformation to value numbers are based on responses from 20 provider and payer Task Force members that responded to the year-end survey. The averages reported are the combined average of each system, and they are not weighted to reflect the organization’s size. For more information please visit: https://hcttf.org
ABOUT THE HEALTH CARE TRANSFORMATION TASK FORCE
Health Care Transformation Task Force is a unique collaboration of patients, payers, providers and purchasers working to lead a sweeping transformation of the health care system. By transitioning to value-based models that support the Triple Aim of better health, better care and lower costs, the Task Force is committed to accelerating the transformation to value in health care. To learn more, visit WWW.HCTTF.ORG.
TASK FORCE MEMBERS
Aetna • agilon health • Aledade • American Academy of Family Physicians • Anthem, Inc. • ApolloMed • Archway Health • Ascension • Atrius Health • Blue Cross Blue Shield of Massachusetts • Blue Cross Blue Shield of Michigan • Blue Cross Blue Shield of North Carolina • Blue Cross Blue Shield of South Carolina • Cambia Health Solutions • CareCentrix • ChenMed • Clarify • Cleveland Clinic • Community Catalyst • ConcertoHealth • Dignity Health • Encompass Health • Evolent Health • Families USA • Geisinger • Heritage Provider Network • HRHCare • Kaiser Permanente • Mark McClellan • Mental Health America • National Health Law Program • National Partnership for Women & Families • OSF HealthCare • Pacific Business Group on Health • Partners Healthcare • patientping • Premier • Remedy • SCL Health • Sentara Healthcare • Trinity Health • Tucson Medical Center • Washington State Health Care Authority • UAW Retiree Medical Benefits Trust
Download the PDF
Media Contact:
Megan Zook
202-774-1578
Megan.Zook@hcttf.org
